Why does the quality of a biological sample matter?
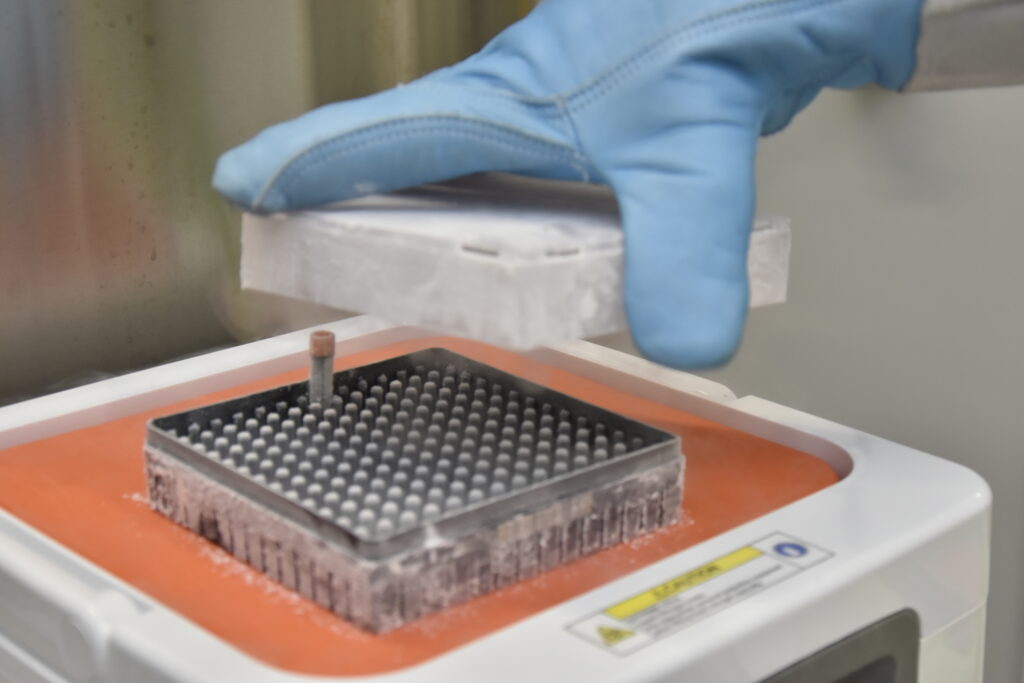
When we think of scientific research or laboratory diagnostics, most of us imagine modern instruments, white lab coats, genetic analyses, AI, or complex statistical models. What we rarely realize, however, is that many of these processes rely on something very fragile and seemingly ordinary, a biological sample. Its quality often determines whether results will be accurate and reliable or misleading and inaccurate.
The sample as the “weakest link in the chain”
A biological sample (blood, tissue, saliva, urine, or cells) carries information about the human body at a specific moment in time. For an analysis to be trustworthy, the sample must reflect the original biological state of the organism as accurately as possible. The problem is that if something goes wrong before the analysis itself, no technology can later “fix” it.
This is why biological samples are often referred to as the weakest link in the experimental chain. If degradation, contamination, or misidentification occurs, the outcome is irreversibly affected.
Where do most errors occur?
Studies show that up to 70% of all laboratory errors arise during the so-called pre-analytical phase, the period covering patient preparation, sample collection, transport, processing, and storage. It is here, rather than during the analysis itself, that the greatest variability occurs.
The most common errors include:
- improper patient preparation (failure to fast, medication use, smoking),
- incorrect labeling or identification of the sample,
- improper collection methods (e.g., hemolysis – damage to red blood cells),
- delayed or improper sample transport,
- temperature fluctuations during handling,
- repeated freezing and thawing.
These and other factors can alter analyte concentrations, cause degradation of DNA, RNA, or proteins, and ultimately lead to false or inaccurate results.
Small errors, serious consequences
Poor-quality biological samples affect not only research projects, but also patients and the healthcare system as a whole.
In scientific research, low-quality samples contribute to the so-called reproducibility crisis, situations where published findings cannot be replicated in other laboratories or with different sample sets. This is not merely an academic problem. It represents wasted grant funding, months or years of researchers’ work, and underutilized expensive technologies.
International studies estimate that billions of euros are spent each year in biomedical research on studies whose findings cannot be reliably verified, often due to poor-quality input samples.
In practice, this means repeated experiments, additional sample collection, repeated analyses, and delays in research projects. Every poor-quality sample generates hidden costs that may not be immediately visible but gradually accumulate. Beyond financial losses, trust is also undermined and researchers lose confidence in their own data, funding agencies question the effectiveness of investments, and the public’s trust in science may decline.
All of this slows the translation of new discoveries into clinical practice and delays the benefits that high-quality research could bring to patients.
Biobanks as guardians of quality
This is where biobanks play a crucial role.
A modern biobank is far more than “a freezer full of samples.” It is a sophisticated infrastructure that ensures:
- standardized collection of biological material,
- controlled processing and long-term storage,
- detailed documentation and traceability of samples,
- systematic quality monitoring.
Biobanks operate according to international standards such as ISO 20387 and European guidelines, ensuring that samples remain comparable across countries and research projects. This is essential for the development of precision and personalized medicine, which depends on large, high-quality, well-annotated datasets.
Sample quality = trust in results
The quality of a biological sample is a silent, often invisible, yet fundamental factor in scientific and clinical success. It affects diagnostic accuracy, treatment efficiency, research effectiveness, and public trust in medicine and science.
If we want modern medicine to advance, it is not enough to invest only in technology. We must also invest in process standardization, staff education, and the quality of biological samples.
Because every reliable result always begins with a reliable sample.
In biobanking, one simple rule applies:
quality preserved today remains valuable in the future.
Proxy Director of BBMRI.sk
RNDr. Romana Záhumenská, PhD.




